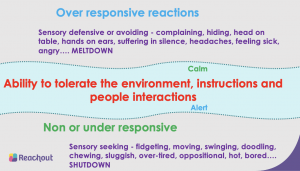
What is a sensory diet and how do I implement one in my busy classroom?
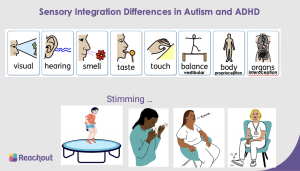
Many autistic children have Sensory Processing Disorders. (And so do children with Down’s Syndrome, ADHD and other or no other conditions). Their sensory systems (as above) can be hyper (over) or hypo (under) sensitive and this affects the way that they understand, perceive and interact with the world around them. It also affects their perception of their own bodies and how they function. And I’m often asked whether the sensory responses can be different on different days, yes, they can. Some sensory responses can be hyper and some hypo in the same person.
Knowing each child’s profile has to be important in order that we can support them and help them understand how to manage their sensory difficulties. These difficulties won’t magically disappear, but what we can do is help a child understand their sensory systems and how they and others can help ‘regulate’ the sensory input so that they can feel calm, alert and manage the stress that it causes.
Sensory Assessments
A sensory assessment should be done by a Sensory-trained Occupational Therapist. If you can get an assessment on the NHS then, congratulations! In many areas, these are as rare as Hen’s teeth. Some CAMHS services do sensory assessments and may have OT input for this and that is great too. Many parents find they have to pay privately for an assessment and there are some excellent OT Sensory Therapists out there. Sometimes assessments are done by people who are not OTs. These might give general guidelines and would certainly not be linked to any specific therapy, but more to environmental accommodations and practical activities at home and school.
For you as a teacher, you may notice that your pupil has sensory avoiding or sensory seeking behaviours. You might have been asked to fill in a questionnaire and you might have had an OT visit your school to observe the child. You might not have noticed anything at school because some children mask their difficulties and the meltdown happens at home. You’ve probably had conversations about sensory processing concerns with parents.
But it is likely that after an assessment you will receive a copy of a report. This report should identify the child’s “Sensory Profile” (their sensory differences and difficulties) and will include a list of suggestions for you to implement in the school day. Often these will start with environmental adaptations. These might be to sit the child in a certain place, make the classroom less overwhelming for the child and add things like a sensory area to your classroom. There will be suggestions for activities, and these lists can be very long!
But…
And therein lies the problem. Some sensory profile reports I have seen have been long, detailed and overwhelming for teachers and teaching assistants (there are some wonderful exceptions with reports that are so easy to work with). The question is always; ‘how do we do all this in our busy classroom and where do we start?”
This is what you can do…
Think of it like this. A sensory diet is like when we eat meals. We have a main meal three times a day, and in between we have snacks. At school, there is one of those main meals and times for snacks between. Sensory activities can be organised, available and monitored with this in mind.
A Sensory Diet
A. The Sensory main meal is a main activity that helps the child regulate their sensory systems so that they feel calm and alert enough to engage with the rest of the school day demands. This could be activities like: (these are examples, there are tons of ideas that might be suggested).
- a break somewhere quiet
- a walk around the schools grounds
- some oral-motor activities
- physical activities such as a sensory circuit
- time wearing a weighted jacket
This may mean that a teaching assistant takes the child out of class for anything between 5 minutes and 1/2 hour whilst the activity takes place. The aim is for the child to have the sensory input or sensory break their system needs so that they have the energy, focus and calmness to continue with the demands of the day.
B. Sensory snacks can happen through the day and should be available or the child to use at any time. These can be – (again, just a few examples)
- headphones to shut out noise overload
- fiddle toys
- knobbly cushions on their chair
- “Chewelry” and oral motor toys
- calming smells
- weighted cushions
(I’d include fidget spinners but they’re mostly banned!! – there are alternatives!)
When choosing what activities to put in place then look at the list you have been given in the report. Speak to parents and the child to gather which activities might already be familiar and working well with the child. Then choose one or two at a time and experiment to see what helps the child and what doesn’t. If it doesn’t, cross it off the list and use another of the ideas. Involve the child and get them to say what they’d like to try (give visual choice boards if needed) and have the child comment on whether the activity makes them feel okay, better and able to join in class learning activities. Try and record what works and what response the child gives so you have evidence for any follow up or review.
​If you timetable the ‘main meals’ in to the child’s visual timetable (see picture) then the child knows it is happening and can build that into their expectations of the day. I have known children who can wait more patiently because they know when the activity is coming. They also need to know that it’s okay to have their ‘snack’ activities WHENEVER they need it. If a child is struggling with noise, then telling them to wait for their headphones isn’t going to help them. They will need to know it is okay to use them whenever they need them. Don’t be worried that some children might use these activities to ‘opt out’ regularly. If the sensory diet is doing its job, then they will feel calmer more often and naturally will join in learning activities. At first it is usual that children use their ‘snack’ activities often. That is good.
The aim of all sensory diets is to help the child learn to “self-regulate”. They should be taught about their sensory systems and how the environment and maybe other people (noise, touch etc) does upset their sensory systems, and that it isn’t their fault. We need to help children know what helps them feel safe, calm and able to engage with the environment, learning activities, and with people. This takes a long-term approach. They are likely to need support throughout their school lives. As a class teacher you are not expected to be an Occupational Therapist. That’s okay. These tips are here to help you implement the advice of a sensory assessment in ways that you as a teacher can organise and manage.

Here are some further reading resources that you might find helpful.
The Out of Sync Child by Carol Stock-Kranowictz
How to support children with sensory processing needs by Lois Addy (LDA)
And to explain sensory processing to children this book is excellent:
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.



 Lynn McCann 2025
Lynn McCann 2025
Thank you. It’s nearly ready for a bit of a tidy up but its a work in progress!
Fabulous site